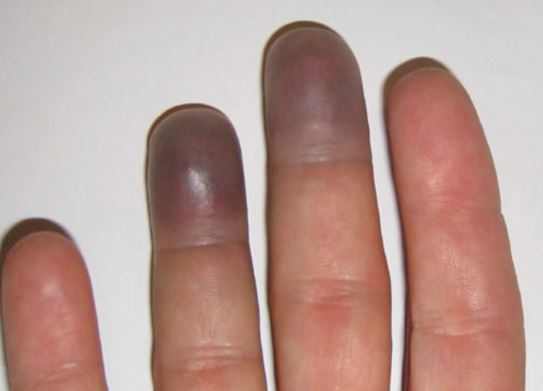
Fingers can turn their color due to various reasons.
Toes and fingertips, too, can change their color depending on the weather and illnesses. Circulation problems, anorexia, and even numbness can cause your fingers to turn purple. Here are the causes and treatments for this symptom.
What do purple fingertips and toes mean?
Having purple fingertips is a medical condition that indicates a deficiency or lack of oxygen in the blood. If your skin is very pale, it might be a sign of blood loss. When the body is deprived of oxygen, the color changes from bright red to dark color. This condition is medically called peripheral cyanosis.
This condition can be observed in the absence of heart or lung failures. Small blood vessels may be restricted and can be treated by increasing the normal oxygenation level of the blood. This rescues the condition. Purple or bluish-colored fingers can be caused by conditions like cyanosis, Reynaud’s phenomenon, and certain medical conditions.
Chronic cyanosis can be a sign of many different lung and breathing problems, including asthma, emphysema, chronic obstructive pulmonary disease, chronic bronchitis, and other respiratory disorders. It also can be a sign of many heart problems, as well as a response to high altitude and overdoses of certain drugs (narcotics, benzodiazepines, and some sedatives).
Raynaud’s disease or phenomenon is most frequent in women, and it leads to numbness and cold when the temperature drops or the sufferer is under stress. The symptoms are caused by poor circulation, the arteries that supply blood to the skin become narrow, and in the long run, restrict the flow of oxygenated blood.
The reasons behind the narrowing of the arteries were unknown as of 2011. There are conditions like rheumatoid arthritis or heart diseases that could precipitate the condition. However, the disease can still occur without these underlying conditions.
The following: Blue, purple fingertips, Dark purple toes, and fingers.
Causes of purple fingers
The following are the possible reasons why your fingertips are turning purple or dark in color.
1. Lupus
This is an autoimmune disorder where the immune system turns against parts of the body it is supposed to protect. This leads to inflammation and damage to various body tissues. Lupus can affect many parts of the body, including the joints, skin, kidneys, heart, lungs, blood vessels, and brain.
A healthy immune system produces proteins called antibodies and specific cells called lymphocytes that help fight and destroy viruses, bacteria, and other foreign substances that invade the body. In lupus, the immune system produces antibodies against the body’s healthy cells and tissues.
Heart and lung involvement often is caused by inflammation of the covering of the heart (pericardium) and lungs (pleura). When these structures become inflamed, you may develop chest pain, irregular heartbeat, and accumulation of fluid around the lungs (pleuritis or pleurisy) and heart (pericarditis).
The heart valves and the lung itself can also be affected by lupus, resulting in shortness of breath. Similarly, the heart is unable to pump enough blood to the extremities while the lungs are unable to oxygenate blood fully.
The causes of lupus are quite unclear. However, there appears to be something that triggers the immune system to attack various areas of the body. To that effect, suppressing the immune system is one of the primary forms of treatment.
Factors that may contribute to the development of lupus include viruses, environmental chemicals, and a person’s genetic makeup. Female hormones are believed to play a role in the development of lupus because women are affected by lupus much more often than men.
2. Cold or numbness
Exposure to cold abnormally reduces blood circulation, causing the skin to become pale, waxy-white, or purple. The disorder is sometimes called “white finger”, “wax finger” or “dead finger.”
Prolonged exposure to extremely cold temperatures (hypothermia) as a result of immersion in cold water or exposure to cold temperature, deep frostbite can cause the fingers to turn blue after some time.
In some sensitive individuals, it happens that after a brief exposure to cold (within seconds) or during periods of stress, one or more fingertips on both sides become pale and numb, then blue then red. The attack may last from several minutes to hours. This is known as Raynaud’s phenomenon or syndrome)
A numbness that results from repeated use of vibration tools like the hammer jack may cause discoloration of the fingertips to white, then bluish. This could take place within 24 hours of exposure to the atmosphere. Discoloration from cold and numbness improves upon exposure to warm temperature or warming.
Another likely cause of discoloration of fingertips is the frostnip. After prolonged exposure to cold, the hands and fingers may become cold, pale (cyanotic), stiff, and possibly numb and tingly. Reheating may lead to annoying pain in the nail beds.
The arterial embolism may also make the fingers suddenly become cold, pale or blue, painful, weak, numb, or tingly. Cramps are likely to develop, and the finger becomes hard to move. If not treated urgently, ulcers or gangrene can develop.
3. Elderly/old age
The aged experience the problem with circulation beginning from the heart. The heart muscles tend to be fatigued and cannot, therefore, pump blood efficiently to the peripheral tissues. The result is a lack of enough nourishment and, therefore, hypoxia (lack of oxygen). In the long run, the color of the fingertips changes to purple or blue.
Similarly, the elderly are likely to encounter reduced elasticity of blood vessels. This makes it hard for oxygenated blood to be pumped effectively to reach peripheral tissues. The color of the fingertips ends up changing to blue or purple.
The lungs are also affected by old age. They are not able to carry out complete oxygenation of oxygen-deficient blood from the heart. The blood that finally reaches the peripheral tissues is either deoxygenated or not adequate for nourishment.
4. Anorexia
Anorexia nervosa is a common eating disorder, which is characterized by the conscious refusal of sufficient calorie intake with an intense fear of obesity and a profound derangement of bodily perception.
This leads to cachexia with consequential endocrine and metabolic disorders, as well as typical skin changes. It involves inadequate calorie intake leading to marked cachexia with metabolic and endocrinological disturbances.
If you have eating disorders, you can suffer from poor circulation of blood around the body as a result of lowered blood pressure. People with this condition suffer from low blood pressure and either a fast or a very slow heart rate (pulse).
When the body is starved, it slows everything down to conserve the limited available energy. For instance, the heart beats more slowly and weakly, to protect its weakened muscle. As a result, blood pressure drops, and the circulation of blood to extremities is reduced. This can cause loss of sensation in the fingers, numb arms, and legs, and some people said their fingers and lips turned blue.
A starved body can’t make as many red cells, white cells, or platelets as a healthy body. Red cells are the ones that carry oxygen around the body in the form of hemoglobin. Without enough red cells, people are anemic, and this leads to a change in color of the skin and mostly the peripheral tissues of the nails.
Your fingernails, as well as hair, both require a protein called keratin to become strong, healthy, and grow at a normal rate. If you suffer from anorexia, then you often do not get enough of the mineral. You are likely to lose hair or develop brittle fingernails. Due to poor circulation, in this case, your fingers turn blue.
5. Circulation problems
Several problems that are associated with circulation like the circulatory shock and blood clot are the main problems that are likely to bring about blue/purple fingers.
Circulatory shock is a medical condition that shows up as low blood perfusion of tissues resulting in cellular injury.
The typical signs of the shock include low blood pressure, rapid heart rate, signs of poor end organ perfusion, and very weak pulses. The outcome of this is that the peripheral tissues, i.e., the fingertips end up getting a low supply of blood rich in oxygen and hence the color change.
Blood clotting, on the other hand, leads to blue/purple fingers because it hinders the efficient flow of oxygenated blood to the extreme tissues. This is because the clot clogs the arteries and veins, thus hindering the smooth flow of blood from the heart through the lungs to the tissues. This leads to deprivation of oxygen to the tissues and hence the change of color.
6. Diabetes and purple fingertips and toes
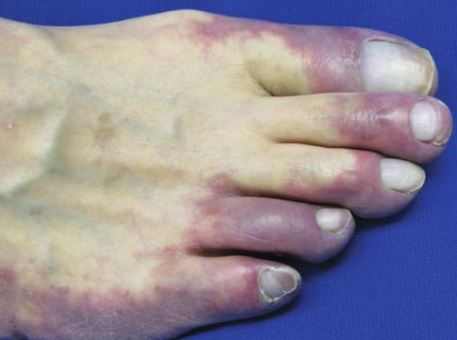
Diabetes has no direct link to purple fingertips, but due to its effects on blood vessels, it could lead to this condition. Other conditions are related to the nerves that supply tissues from time to time.
First of all, it comes with diabetic neuropathies (damage to the nerves), which are a family of nerve disorders that lead to numbness and sometimes pain and weakness in the hands, arms, feet, and legs. Neuropathy can also cause problems in your digestive system, heart, and sex organs.
High blood glucose causes hardening of the arteries (atherosclerosis), which can lead to a heart attack, stroke, or poor circulation in the peripheral tissues and, most likely, the fingertips.
Apart from that, diabetes leads to damage to small blood vessels such as capillaries (called microvascular disease). These are the fundamental structures that supply the tissues at the fingertips.
High blood glucose, as seen in diabetics, also thickens capillary walls, makes the blood stickier and can cause small blood vessels to ‘leak’. Together, these effects reduce blood circulation to the skin, arms, legs, and feet.
According to some medical theory, it has been noted that molecules known as Advanced Glycation end products (AGEs) are involved in the damage that is sustained by blood vessels. AGEs are the result of fats and proteins that have become glycated through exposure to glucose. Researchers have concurrently found higher levels of AGEs in the blood of people who have developed diabetic complications.
High blood glucose levels over time can lead to increased deposits of fatty materials on the insides of the blood vessel walls. These deposits may affect blood flow, increasing the chance of clogging and hardening of blood vessels.
Purple fingers after surgery
The outcome of surgery can determine how you will look for the remaining part of your life. If you undergo hand surgery, and it happens that there is an interference with the blood supply, then you are likely to face a condition that leads to purple fingertips.
This, in most cases, happens when a surgery damages the nerves and blood vessels that supply the hand. If the blood vessels are damaged, then it comes out that the tips of fingers will not get enough perfusion and hence low oxygen. This leads to blue/purple fingers. A correction should be made immediately such an occurrence is noticed to limit further complications.
Treatment
The first approach to treatment and management of this condition constitutes basic and simple techniques that help relieve the symptoms and likelihood of the condition. You should:
- Keep your hands and feet warm. Warm gloves, socks, and shoes are essential when you are out in cool weather. We recommend HeatMax Hot Hands Warmer (Check price on Amazon)
- Keep your whole body warm, not just your hands and feet. Although your hands and feet are the most important, symptoms are less likely to occur if you keep your entire body warm. So, wrap up warmly before going into cooler areas, such as outside on cold days. For example, wear hats and scarves in addition to warm clothes.
- Ensure you put gloves on when you are warm before going into colder areas. Ideally, keep gloves, socks, and headgear in an airing cupboard or near a radiator so they will be warm when put on.
- If you have severe symptoms or symptoms that are easily triggered, then portable heat packs and battery-heated gloves and socks are useful. Your pharmacist or local medical supplier may also be able to advise accordingly.
- Try not to touch cold objects. For example, use a towel or gloves when removing food from the freezer or working with cold food.
- Many health experts recommend regular exercise. Exercise your hands and feet frequently to improve the circulation.
- When some of the symptoms develop, warm the affected hands or feet as soon as possible. Soaking the hands or feet in warm running water is a good way to get warm (but take care that the water does not become too hot, or lose its heat and become cool)
- An attack should not be ignored. A few simple actions can lessen its length and severity. When symptoms occur, take fast action to warm the affected area as soon as possible (e.g., by moving to a warm environment or by immersing hands or feet in warm [not hot] water).
- Stress and emotional upset can precipitate attacks, so avoiding stressful situations, and learning relaxation techniques can be beneficial.
- Stop smoking. Nicotine causes vasoconstriction, and smoking can make symptoms worse (smoking a cigarette can cause a reduction in fingertip temperature of 2–3C).
- Caffeine can trigger symptoms. Avoid beverages containing caffeine for a few weeks to see if symptoms improve.
In case the above approaches fail to give appropriate results, there is a need for treatment using drugs. This approach is the most effective and works within a very short time. The break down is given below.
Calcium channel blockers:
These are the most typical and first choice in the treatment of purple skin color conditions. They are suitable when prescribed, although there is limited evidence of their efficacy. An analysis carried out found that calcium channel blockers reduced the frequency of ischemic attacks by an average of 2.8–5.0 per week and reduced severity by 33 percent.
Nifedipine
Particularly, nifedipine is the most commonly used and has the most evidence of benefit. It is the only calcium channel blocker licensed to treat purple skin color conditions. It relaxes vascular smooth muscle, causing peripheral vasodilation. A starting dose of 5mg three times a day is recommended. It is thereafter adjusted, according to response to up to 20mg three times daily. It, however, presents side effects that include: flushing and headache (these are most significant in the early days of dosing and often decrease with continued treatment) and ankle edema.
The antihypertensive (works on reducing blood pressure) properties of nifedipine can mean that it is not suitable for patients with low blood pressure. It should also not be used within a month of a heart attack, or in people with heart failure. Since sufferers are commonly young women, nifedipine’s contraindication in pregnancy and breastfeeding should be kept in mind. Patients with severe symptoms take nifedipine regularly, but others only take it during the winter months when their symptoms are at their worst.
The modified release nifedipine preparations are not licensed for Raynaud’s phenomenon, but they may be better tolerated.
Other dihydropyridine calcium-channel Blockers that include amlodipine, felodipine, and isradipine) have shown some benefits in small studies.
On the contrary, verapamil and diltiazem are not recommended because their main site of action is on myocardial (heart) tissue, and they have a lesser effect on the peripheral vasculature (tissue).
Licensed drugs
Other peripheral vasodilators such as naftidrofuryl and inositol nicotinate are sat times used but are of uncertain value. They may have applications in those who are intolerant to calcium antagonists.
Pentoxifylline, prazosin, and moxisylyte are also licensed for use in Raynaud’s but are not established as being effective.
Unlicensed drugs
Angiotensin-Converting Enzyme inhibitors (even though some cause Raynaud’s symptoms) and angiotensin-II receptor antagonists may provide some small benefits in this condition. There is no evidence to suggest that they are more effective than the calcium channel blockers.
Serotonin reuptake inhibitors
Some serotonin reuptake inhibitors, like fluoxetine, are useful. Serotonin causes vasoconstriction, so by reducing serotonin levels, some vasodilation is achieved. Results to date have been promising, but more evidence is needed.
Prostaglandins
Prostaglandin E1 and prostacyclin are potent vasodilators and inhibit platelet aggregation. The prostacyclin analog-like iloprost (with a half-life 10 times that of prostacyclin) has been used on a named-patient basis to manage severe Raynaud’s symptoms, particularly in patients with scleroderma.
It has been shown to reduce both frequency and severity of attacks and been used in the treatment of fingertip ulcers associated with Raynaud’s symptoms. It is usually given as a six-hour intravenous infusion at a dose of 2ng/kg on three consecutive days.
Sildenafil
The micro- and macrovascular dilating properties of sildenafil have shown promising results in accelerating digital ulcer healing rates in scleroderma patients with Raynaud’s symptoms. In a trial, 50mg twice a day of sildenafil, given for four weeks, gave a definite improvement of symptoms.
Food supplements
Some food supplements have been proposed as being beneficial in Raynaud’s phenomenon, including anti-oxidants and fish oils.
The World Health Organization has recommended the use of Ginkgo biloba in the treatment of Raynaud’s. Ginkgo biloba, 120mg three times a day, was effective in reducing the number of attacks of Raynaud’s. The supplement was well tolerated and accepted by patients.
Surgery
For patients with severe symptoms and who do not respond to other treatments, a sympathectomy -cutting the nerves that supply the affected part may be performed.
What of the crises?
In the event of an acute ischemic crisis (i.e., where there is a danger of the loss of tissue), you should be directed to the hospital immediately.
Treatment includes vasodilation (e.g., intravenous infusion of iloprost, oral nifedipine), pain relief (e.g., lidocaine or bupivacaine), surgery and anticoagulation (e.g., low-dose aspirin or short-term heparin if there is persistent critical ischemia or occlusive disease of large arteries).