COVID-19 outbreak is still an evolving situation. As research is still ongoing the vaccines available so far can differ with time. Therefore what is mentioned in this article may change in the future.
According to CDC (Centers for Disease control), the COVID-19 virus spreads mainly from person to person through respiratory droplets, from an infected person by coughing and sneezing. Virus gets in mainly by inhalation. People are most contagious when they are symptomatic. However, the virus can spread even during the incubation period that is around 14 days. There is also a high possibility to get infected by touching an object or a surface that is contaminated by the virus and touching your own nose and mouth.
Symptoms usually appear 2-14 days after exposure. Fever, cough (mainly dry cough) and shortness of breath are common symptoms, while headache, body aches and sore throat may also occur. Those who suffer from immunity disorders, elderly and those with other medical conditions such as ischemic heart disease, hypertension and diabetes are considered high risk for getting infected and to develop severe illness.
COVID-19 is a virulent virus that causes a higher death rate than other viral infections or influenza. It may spread easily in communities. COVID-19 respiratory disease was declared a Pandemic by the WHO on 11th of March 2020.
COVID-19 can give you serious life threatening complications. There is no way to know how this virus will affect you.
According to the UN chief Antonio Gutteres, “After a year of chaos, vaccines provide some light at the end of the tunnel”. However, with various different brands of vaccines being introduced by many leading biopharmaceutical companies, there surfaced some serious conflicts of opinion.
The first mass vaccination program was started in early December 2020. Vaccination is the safest and the most effective way to help you build protection against the COVID-19 virus. WHO has issued EUL (Emergency Use Listing) for several vaccines so far.
What is meant by Emergency use listing (EUL)?
EUL procedure assesses the suitability of any novel product during public health emergencies. The objective of the EUL is to make vaccines, medicines and diagnostics available as soon as possible to address health emergencies. While making sure that stringent criteria of quality, safety and efficacy are adhered to. This assessment weighs both the pros and cons. That is the threat posed by the health emergency as well as the advantage by using the product against possible risks. When it comes to EUL of a vaccine, independent experts and WHO teams consider all the evidence on vaccines, results from clinical trials and plans for monitoring its use. Once a vaccine has been listed for emergency use, WHO engages its regulatory networks to monitor the benefits and risks of the vaccine up to date.
World Health Organization issued an EUL first for Pfizer COVID-19 vaccine (BNT162b2) on 31st December 2020. Then EULs were issued for 2 versions of AstraZeneca /Oxford COVID-19 vaccine by the WHO. They are manufactured by the serum Institute of India and SKBio.
Once vaccines are demonstrated to be safe and efficacious, the national regulators must authorize it to be manufactured to exact standards and distributed. All approved vaccines require proper distribution with temperature control and rigorous stock management.
What are the vaccines approved by the FDA for the use in the US?
There are 3 COVID-19 vaccines that are FDA approved for the use in the US – Pfizer, Moderna and Johnson and Johnson (Janssen). All 3 types available in the US have been tested for safety and efficacy (while continuously monitored for safety) and all 3 are shown to be highly effective. While preventing infection, they are effective at preventing serious illness and complications due to COVID-19.
Due to the limited supply of the vaccines you should get whichever vaccine (out of these 3) that is offered to you. All 3 types help to prevent hospitalization and death from COVID-19. They also prevent you from getting moderate to severe COVID-19 illness.
Comparing the efficacy of COVID-19 Vaccines used in US
Based on the evidence from the clinical trials;
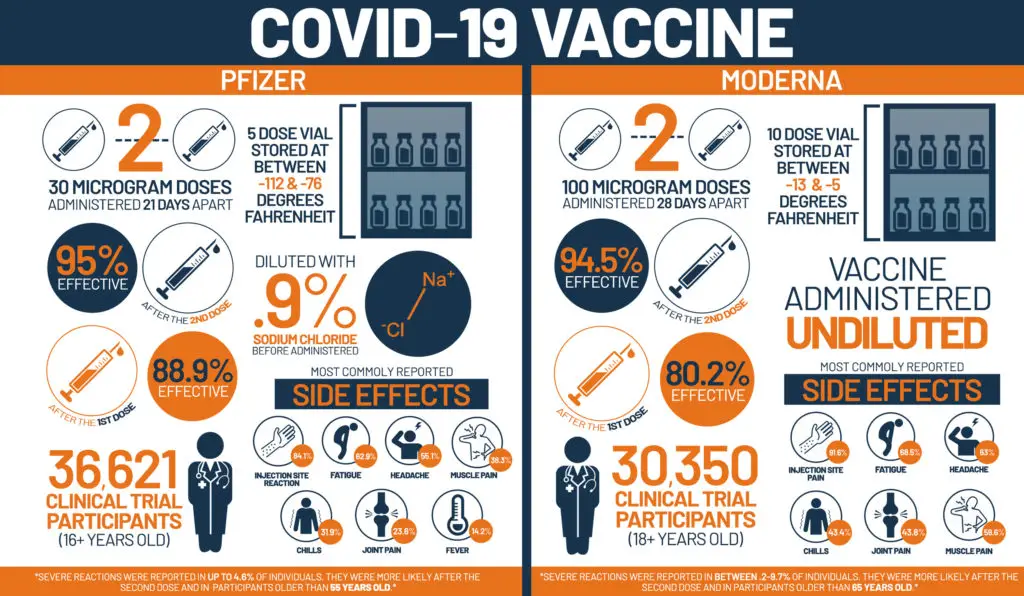
- The Pfizer two dose COVID vaccine is 95% effective
- The Moderna two dose COVID vaccine is 94.1% effective
The first dose provides around 70% protection against COVID-19 infection. The second dose is considered as a booster dose. It further increases the immunity and gives up to 95% protection against this deadly virus. The second dose is recommended to be given 10 to 12 weeks after the first dose.
- Johnson and Johnson single dose vaccine is 63.3% effective at preventing COVID-19 illness.
All eligible persons must be vaccinated. Currently ample scientific evidence is available for vaccinating everyone who are above 18 years of age, unless there are any contraindications.
Pfizer-BioNTech COVID-19 Vaccine
This is the first approved vaccine by the WHO for emergency use. It is a mRNA vaccine that is safe and effective. Since it was the first approved vaccine priority was given to health workers with high risk of exposure, followed by older adults before immunizing the rest of the population. When decision making is done whether to vaccinate, testing for prior infection is not recommended.
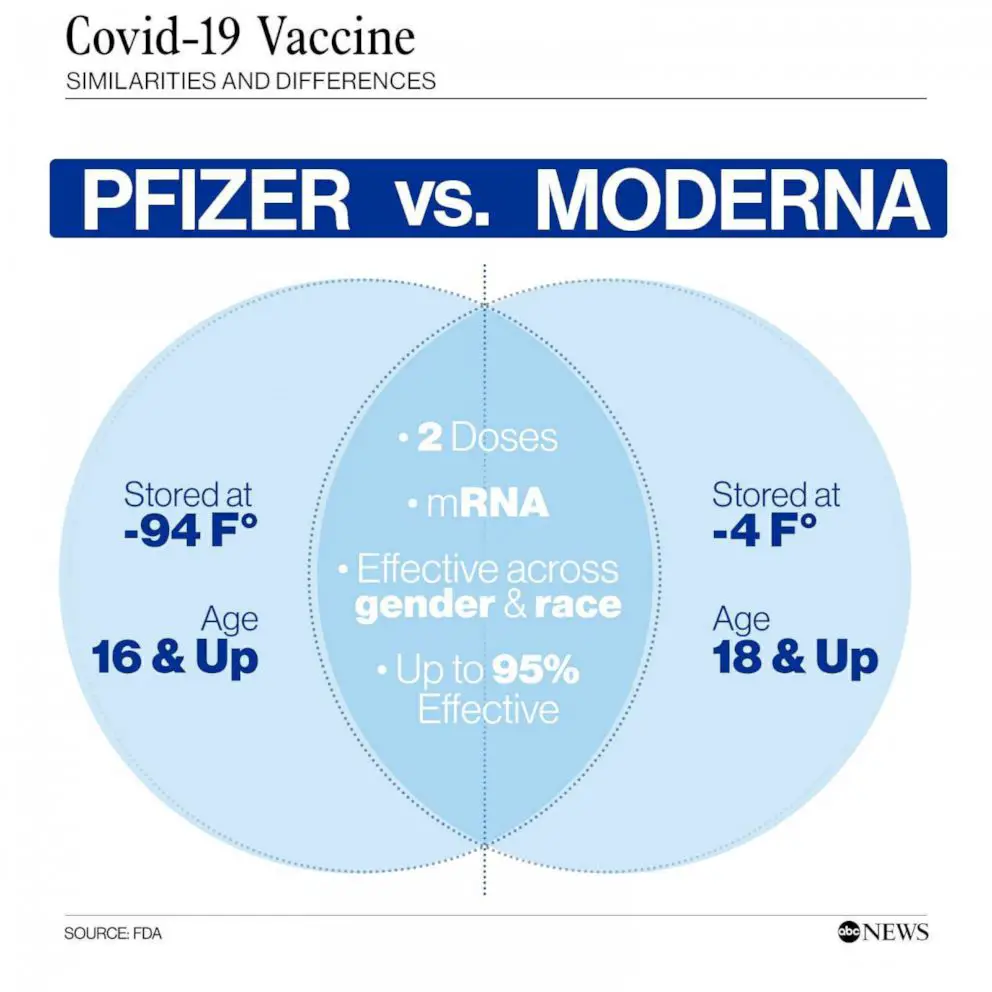
The vaccine should not be administered to persons younger than 16 years of age pending the results of further studies.
Protection or immunity will start to develop 12 days after getting the first dose of the Pfizer vaccine. However, full protection requires two doses. 2nd dose is recommended to be administered with a 21 – 28 day interval.
Pfizer vaccine has to be stored at -70C for up to 10 days to maximum 30 days unopened. Pfizer has temperature controlled thermal shippers utilizing dry ice to maintain this temperature. In hospital setting, this vaccine can be stored for 5 days at 2-8 C.
Who should not be vaccinated with Pfizer?
- Those who are pregnant and breast feeding – they are not included in the vaccination campaign because there is no long term safety data
- Children less than 16 years
- People who have an ongoing fever related illness
- Patients with a history of severe allergies
Moderna COVID-19 (mRNA – 1273) vaccine
Priority given to health workers at high risk of exposure and older adults for vaccination. Those of you who were infected with the virus can differ your own vaccination for up to 6 months from the time of infection.
Moderna vaccine can be offered to breast feeding women in the recommended priority group such as health workers. Following vaccination no need to discontinue breast feeding.
Pregnant women with high risk of exposure may be vaccinated in consultation with their health care provider.
Very frail elderly people with an anticipated life expectancy of less than 3 months can be exempted from the vaccine after individual assessment.
Use of the Moderna vaccine is recommended at a schedule of 2 doses (100 Micrograms, 0.5ml each) 28 days apart. If necessary this interval between the 2 doses can be extended to 42 days. Immunity from the Moderna vaccine starts 14 days after the 1st dose.
Moderna vaccine can be stored at regular freezer temperature at -20 C for up to 6 months. After thawing it can be kept in the refrigerator at 2 – 8 C for 30 days. It can be kept at room temperature for up to 12 hours.
Both Pfizer and Moderna vaccines are mRNA vaccines. This means part of the COVID-19 virus’s genetic code is injected in to the body that triggers the body to start making viral proteins, but not the full virus. This is enough to train our immune system to attack.
Janssen COVID-19 Vaccine (Johnson and Johnson)
This vaccine is administered as a single dose. It is given as an intra- muscular injection. Age limit is 18 years and older. Children, pregnant women and breast feeding mothers are not candidates for Janssen COVID-19 vaccine.
There is no data to support the use of Janssen COVID-19 vaccine to complete a vaccination series initiated with another type of COVID-19 vaccine. Administer this vaccine alone. Separate this vaccine by 14 days before and after the administration of other vaccinations.
Storage of Janssen vaccine – this can be refrigerated at a temperature of 2 – 8 C.
What are the factors common to all COVID-19 vaccines?
- After each vaccination, observation should be done for at least 15 minutes for any reactions
- Same product of the vaccine must be used for both doses.
- Even after vaccination with any type of vaccine, safety measures like social distancing, wearing masks and hand washing should be adhered to.
Can people with chronic medical illnesses be vaccinated?
Patients who suffer from long standing lung diseases like asthma and COPD, heart disease, Diabetes, kidney disease, arthritis and those with chronic liver disease should undergo vaccination. These disease conditions put them at a higher risk of getting serious complications from COVID-19 infection. Therefore those with long standing illnesses should be prioritized and given the vaccine. Those who lead unhealthy life styles like smoking and chronic alcohol consumption should also receive the vaccine. There are studies being done among smokers that indicate an additional risk of developing COVID-19 related complications.
Those who are on warfarin (a blood thinning drug) can get immunized if their INR test value is less than 3. It is not necessary to stop warfarin before vaccination. If the INR value is higher than 3, opinion should be seeked from a medical specialist prior to getting vaccination due to the possibility of bleeding.
Patients who are immune-compromised or those taking immunosuppressive medications like cancer chemo therapy, radio therapy, prednisolone, Azathioprine, dexamethasone, Cyclosporin or tacrolimus can get vaccinated without any issues by any type of recommended vaccine.
Lot of queries are there whether the COVID-19 vaccines itself can cause the actual disease. But there is no such possibility because none of these vaccines contain the virus. The vaccines also cannot cause the PCR test to become positive.
Can you get vaccinated if you had a previous COVID-19 infection?
If you were already infected with COVID-19 and deemed cured, you should wait 2 to 4 weeks following recovery before getting any type of COVID vaccine.
What are the benefits of being vaccinated against the COVID-19 infection?
There are several benefits which you will get following vaccination. Following benefits are the most important.
- Vaccination will reduce the chance of contracting the disease as a result of developing immune response to the virus. Developing immunity by vaccination means there is reduced risk of developing the illness and its consequences. This immunity will help you to fight the virus, if you are exposed.
- Vaccination will decrease the severity of the disease as well as the need for hospitalization by 95%.
If this is put in to simple terms, the chance of acquiring a deadly illness is brought down by vaccination. If a vaccinated person gets infected, there will be only a remote possibility of severe complications and death.
- Getting vaccinated can also protect the people around you. If you are protected from getting the infection and from the disease, you are less likely to infect someone near you. This is very important in protecting people of increased risk for severe disease from COVID-19, such as health care workers, elderly and patients with other medical conditions.
These benefits are seen in all approved vaccines for emergency use.
What are the common side effects of COVID-19 vaccines?
- Pain at the injection site
- Fatigue
- Muscle aches and pains
- Nausea and vomiting
- Headache
- Fever and chills
Most of these side effects will occur within 1 – 2 days following vaccination. They are usually mild to moderate in severity and commonly lasts only for 1 to 2 days.
Side effects after the 2nd injection can be more severe than the ones you experienced after your first dose. These side effects are usual signs that your body is gradually building protection. These side effects should go away within a few days.
When should you seek help?
Above mentioned simple side effects and even fever with chills are signs that your body is building immunity. Seek help from your doctor if;
- The site of injection becomes red and tender and worsens after 24 hours
- Worrying side effects that do not go away within a few days
- Dial 911 if you or someone develop any features of a severe allergic reaction or anaphylaxis such as shortness of breath, feeling faintish, clammy skin, fast heartbeat, wheezing, collapsing or lose consciousness
What can you do to reduce these side effects?
- If you develop fever and body aches you can take acetaminophen (Tylenol) in usual dosage.
- You should hydrate yourself well by drinking water and other healthy liquids.
- Carry out the routine activities without hindrance.
- You can take a bath/ body wash after the vaccination
Is there a relationship between experiencing side effects and the degree of protection?
There is no such connection between side effects and the efficiency of the vaccine. However, you should continue to comply with wearing masks, hand washing and social distancing even after receiving both doses of the vaccine to assure further protection.
Can patients with allergies get the vaccine?
Patients with known allergies are advised to obtain the COVID-19 vaccine under medical supervision. They should be given the vaccine in a health care facility. This is considered when giving any type of COVID vaccine. Past history of severe allergies is a contraindication for vaccination.
What are the other types of COVID-19 vaccines used in other countries?
Several other vaccines have been developed and authorized for emergency use in other countries apart from the 3 vaccines used in US.
Oxford /AstraZeneca COVID-19 vaccine
This vaccine is made from a genetically engineered virus. Priority is given for health care workers, those with comorbidities and elderly. Vaccination is given for people who are 18 years and older. For pregnant and breast feeding women, especially those at a high risk of exposure may be vaccinated in consultation with their health care provider. They may receive the vaccine if the benefit outweighs the potential risk of vaccination.
Recommended dosage is 2 doses with an interval of 8 to 12 weeks. This is an intra-muscular injection.
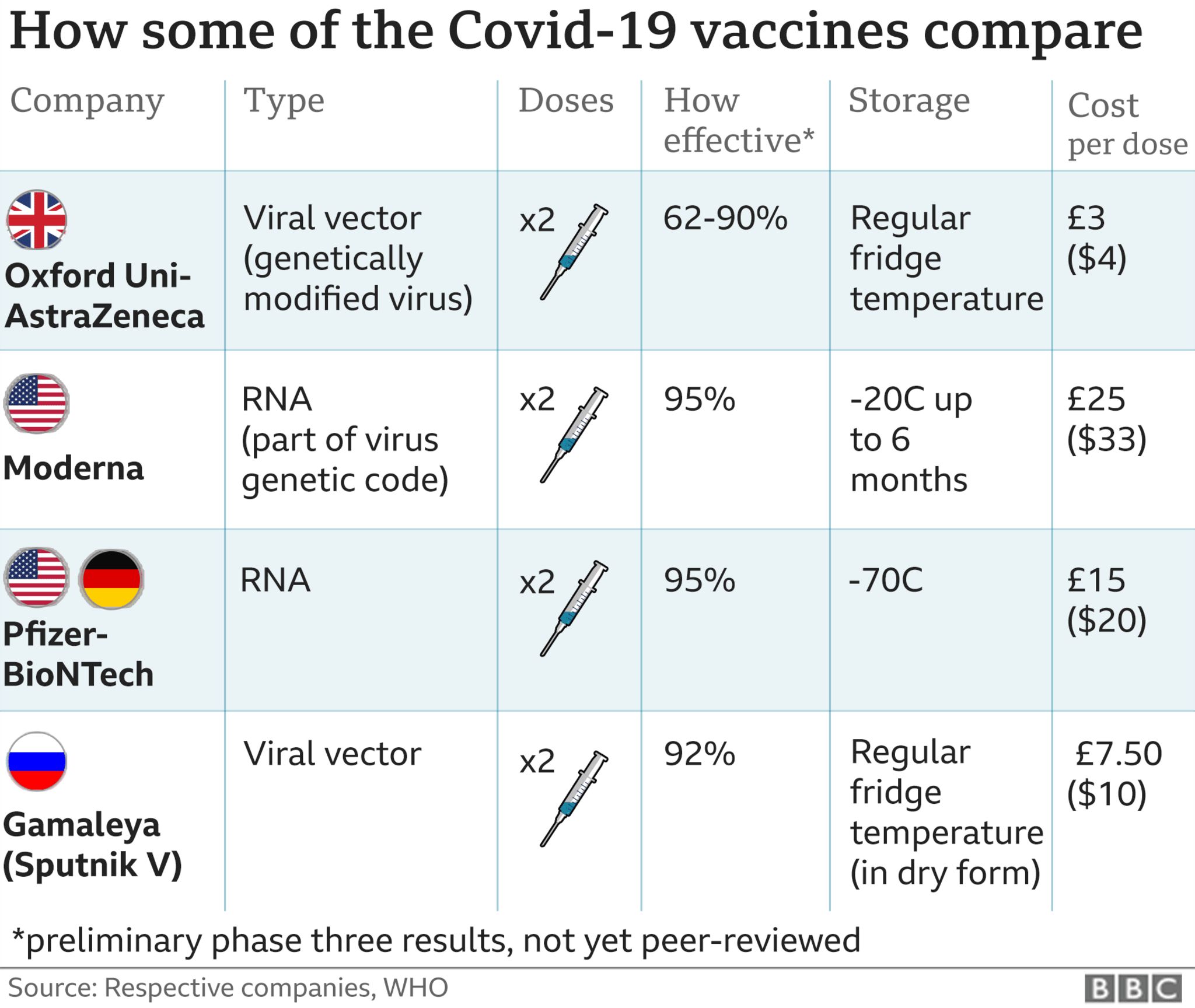
2 versions of Oxford AstraZeneca vaccine have been listed for emergency use by WHO – produced by AstraZeneca – SKBio (Republic of Korea) and the Serum Institute of India. AZD 1222 vaccine has an efficacy of 63% against symptomatic COVID-19 infection. Larger dose intervals within 8 to 12 weeks range is known to be associated with greater efficacy of the vaccine. No data is available related to the impact of the vaccine on transmission and viral shedding.
The storage of Oxford/ AstraZeneca vaccine is at 2 – 8 C.
Sputnik V COVID-19 Vaccine (Gam-COVID-Vac)
This vaccine is developed by Russia’s Gamaleya National Centre of Epidemiology and Microbiology.
It is recommended that 2 doses should be administered 21 days apart.
There are 2 versions of the Sputnik Vaccine. When it comes to storage, one type needs to be freezed at -18 C while the other can be stored at 2-8 C in a standard refrigerator.
Russia’s Sputnik V has a 92% efficacy.
Novavax COVID-19 vaccine (NVX – Co V2373)
The clinical trials were conducted in the United Kingdom. This vaccine is also effective against both UK and South African variants of COVID -19.
It is made from a purified protein encoded by the genetic sequence of the virus. However, it cannot cause infection nor can it replicate.
Novavax COVID-19 vaccine is found to have an efficacy of 89.3%.
This vaccine can be stored at 2 – 8 C in a standard refrigerator.
China’s COVID-19 Vaccines – Sinovac and Sinopharm
These vaccines use killed viral particles to expose the body’s immune system to the COVID virus, without risking a serious disease response.
Both these vaccines can be stored in standard refrigerator at 2 – 8 C.
Vaccines which can be stored in standard refrigerators are a lot more useful for developing countries. Because they do not have adequate storage facilities for large amount of vaccines in freezers as well as facilities to maintain the cold chain at very low temperatures.
Efficacy of the Chinese vaccines vary from 50 – 70%.
Are there certain vaccines which are banned or being suspended in countries?
AstraZeneca’s vaccines are banned in several countries (so far 18 countries) over possible side effects.
Ex: Sweden, Germany, France, Italy, Spain
Few people have died after receiving the AstraZeneca shot. It is unclear whether the reported blood conditions caused their deaths. AstraZeneca COVID-19 vaccines have been suspended while investigations are still being carried out regarding its side effects. Therefore, this vaccine is not yet authorized for emergency use in the US. Still there is no evidence that this vaccine causes blood clots.
Some countries ban vaccines being stuck between the pandemic and politics. Although governments around the world are desperate for COVID vaccines, some countries are not only refusing vaccines produced by their rivals but officially banning them in their countries.
Ex: Ukraine banned Russian Sputnik V, but ordered Sinovac from China
Iranian government has banned all US and British made vaccines and approved Sputnik V.
Taiwan banning Chinese vaccines
Many governments battle publicly for limited doses and even accuse other countries of hoarding. Yet politics play a role which seems a bigger issue than the safety obtained from getting their people vaccinated.
Can you travel following vaccination?
Countries have different travel policies. If you wish to travel after getting vaccinated, your travel dates should start 14 days after receiving the 2nd dose. However, if you show potential symptoms of infection, you should avoid traveling. People still can contract the virus even after being fully vaccinated.
Take home message…
An immunized person can have the disease without symptoms because there is no 100% protection from any of these vaccines. There is also a possibility of them spreading the virus to healthy individuals. It takes time to develop the immunity. Therefore, it is of paramount importance that all of you who are vaccinated should adhere to and continue safety precautions regardless of whichever vaccine you received.
Safe and effective vaccines will be definitely a game changer. Being vaccinated doesn’t mean that we can avoid or throw precautionary health measures to the wind, because we then put ourselves and others at risk.
References:
https://vaccinateyourfamily.org/covid19faq/
https://www.ema.europa.eu/en/news/ema-starts-rolling-review-sputnik-v-covid-19-vaccine
https://www.bbc.com/news/world-asia-china-55212787
https://ir.novavax.com/news-releases/news-release-details/novavax-covid-19-vaccine-demonstrates-893-efficacy-uk-phase-3
https://www.washingtonpost.com/world/2021/02/03/ukraine-russia-iran-vaccines/