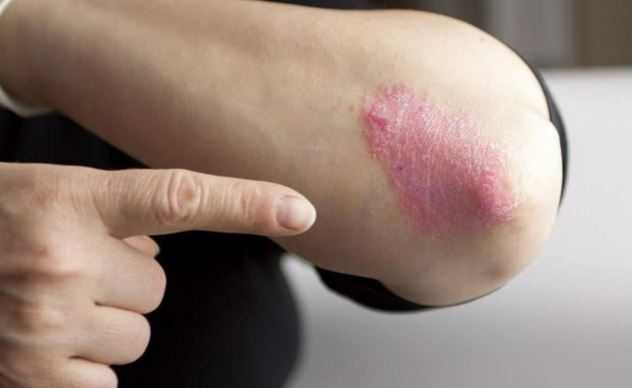
A rash on elbows and knees, legs, forearms, knuckles and wrists can be caused by scabies, eczema and even lupus. When sick with psoriasis, celiac disease or some virus infections, you can also get a severe rash on your elbows. The rash can be itchy, turn red and won’t go away. Here are the causes and treatments for bumps and rashes on inner elbows.
An itchy, blistering, burning skin rash, dermatitis herpetiformis (DH) is a difficult condition to live with. The rash and itching occur on the elbows, knees, scalp, back, and buttocks.
This rash on elbows likely indicates an allergy to gluten, which is a more serious underlying condition that’s also known as celiac disease. DH is sometimes called Duhring’s disease or gluten rash. People who have this condition need to maintain a strict gluten-free diet.
The causes of this condition vary and as such the treatment methods will vary according to the cause. This article will explore the various causes and treatment methods for this condition
Elbow Rash Causes
What causes rash on elbows and knees? Psoriasis and eczema are the most common causes of skin rashes. However, bumps and small dots or blisters can also be caused by diabetes, celiac disease, lupus, etc. Below is a detailed discussion of the possible causes of elbow rash on your skin.
1. Elbow eczema and Psoriasis
Eczema is a general term that describes several different conditions in which skin is inflamed, red, scaly, and itchy. Eczema is a common skin condition, and atopic dermatitis (also called atopic eczema) is one of the most common forms of eczema.
The appearance of eczema can vary from person to person. In adults, eczema occurs most frequently on the hands and elbows, and in “bending” areas such as the inside of the elbows and back of the knees. In young children, eczema is often seen on the elbows, knees, face, neck, and scalp. Signs and symptoms of atopic eczema include:
- Itchiness
- Skin redness
- Dry, scaly, or crusted skin that might become thick and leathery from long-term scratching
- Formation of small, fluid-filled blisters that might ooze when scratched
- Infection of the areas where the skin has been broken
Unpredictable and irritating, psoriasis is one of the most baffling and persistent of skin disorders. It’s characterized by skin cells that multiply up to 10 times faster than normal.
As underlying cells reach the skin’s surface and die, their sheer volume causes raised, red plaques covered with white scales. Psoriasis typically occurs on the knees, elbows, and scalp, and it can also affect the torso, palms, and soles of the feet.
The symptoms of psoriasis vary depending on the type you have. Some common symptoms for plaque psoriasis — the most common variety of the condition — include:
- Plaques of red skin, often covered with loose, silver-colored scales; these lesions may be itchy and painful, and they sometimes crack and bleed. In severe cases, the plaques of irritated skin will grow and merge into one another, covering large areas.
- Disorders of the fingernails and toenails, including discoloration and pitting of the nails; the nails may also begin to crumble or detach from the nail bed.
- Plaques of scales or crust on the scalp
2. Diabetes
Diabetes can affect every part of the body, including the skin. In fact, such problems are sometimes the first sign that a person has diabetes. Luckily, most skin conditions can be prevented or easily treated if caught early.
Some of these problems are skin conditions anyone can have, but people with diabetes get more easily. These include bacterial infections, fungal infections, and itching.
Other skin problems happen mostly or only to people with diabetes. These include diabetic dermopathy, necrobiosis lipoidica diabeticorum, diabetic blisters, and eruptive xanthomatosis.
The culprit in fungal infections of people with diabetes is often Candida albicans. This yeast-like fungus can create itchy rashes of moist, red areas surrounded by tiny blisters and scales.
These infections often occur in warm, moist folds of the skin. Problem areas are under the breasts, around the nails, between fingers and toes, in the corners of the mouth, under the foreskin (in uncircumcised men), and in the armpits and groin.
3. Celiac Disease
Dermatitis Herpetiformis is a skin manifestation of celiac disease and is part of the abnormal immune response to gluten.
Dermatitis herpetiformis (DH) is a severe, itchy, blistering skin rash. DH is a chronic condition that is considered to be the skin form of celiac disease. Not all people with celiac disease develop DH.
The rash usually occurs on the elbows, knees, and buttocks and it is typically symmetrical, meaning it appears on both sides of the body. When the rash goes away, which it often does spontaneously, it may leave brown or pale marks on the skin where pigmentation is lost.
Skin contact with gluten-containing foods and products has not been shown to cause outbreaks.
Who Can Get Dermatitis Herpetiformis?
- About 15-25% of individuals with celiac disease experience DH
- DH affects more men than women
- DH generally starts in adulthood. It’s not common to see DH in children, but it can occur
Only about 20 percent of people with DH have intestinal symptoms of celiac disease, however biopsies show that 80 percent have some degree of damage to the small intestine, especially if a high gluten diet is maintained.
4. Rash on elbows from tanning bed
For those of you that are just experiencing a rash caused by a tanning bed or tanning salon, this is the most likely cause.
Most rashes are caused by basically overdoing it on the tanning bed, and you skin is receiving more UV radiation than it can generally handle. This causes what is called an overdose on your skin, because you skin, or more specifically the melanin on the skin, can’t absorb the radiation coming from the tanning bed fast enough.
The excess causes the rash that appears on your skin.
5. Dry Skin and rash around your elbows
This is another common cause of tanning bed rash. The heat and the hot light from the tanning bed quickly dries out your skin. This can cause a rash and is also a common cause of the itching on the skin that can you sometimes get after using tanning beds.
6. Light Sensitivity Disorder
The one cause of tanning bed rash that you can’t do anything about. Some people have what is called a light sensitivity disorder, this is basically where the lights within a tanning bed cause a reaction within the skin, it is almost like an allergy.
Unfortunately, there is nothing that you can do about this, if you have the disorder/allergy then you have the disorder. You basically need to make a decision whether the tanning is it worth it for you if you have this disorder.
If you can tolerate the rash, then great, you are fine. But if you can’t stand the rash then you should stop tanning, as this is the only thing that will make it go away.
7. Sun Exposure in summer
In the setting of developing this rash on sun-exposed areas, solar dermatitis is the most common diagnosis. Solar dermatitis (or sun rash) can have many different causes.
Most commonly among children, this is idiopathic (no clear cause), and can be avoided by avoiding exposure to sunlight or a higher SPF level of sunscreen.
There is a rare form of allergy to sunlight called “solar hives” or “solar urticaria” that can be an allergic-type reaction to sunlight, but this is also exceedingly rare. Solar dermatitis in and of itself does not pose any long-term harm, but excessive sun exposure at a young age can be harmful.
8. Gluten Allergy and Skin Rashes
While the term gluten allergy is widely used to describe a variety of symptoms, it is not a meaningful or accurate term by itself. You may suffer from a wheat allergy, celiac disease or non-celiac gluten sensitivity (NCGS), but a gluten allergy is not an available diagnosis.
Instead, gluten allergy is often used as a blanket term for these three other conditions.
In addition, a gluten skin rash might be a manifestation of an allergy or an autoimmune response that involves some kind of gluten intolerance not diagnosed as celiac disease or a wheat allergy.
To understand how these conditions are separate, differentiate them by how quickly symptoms manifest after exposure. An allergy is a type 1 hypersensitivity.
This means you will react either immediately or almost immediately after exposure. It also involves IgE (Immunoglobulin E) rather than the antibodies present with diagnosed celiac disease symptoms.
Symptoms of wheat allergy include:
- Nausea and vomiting
- Diarrhea
- Irritation of the mouth and throat
- Hives and rash especially on the folded areas on the body eg rash on elbows.
- Nasal congestion
- Eye irritation
- Difficulty breathing
9. Lupus and elbow rashes
Lupus symptoms are wide and varied. Lupus may strike aggressively as an acute and severe illness, or grumble on undiagnosed for many years. Alternatively, Lupus may appear as a transient disease.
Earlier diagnosis and more effective treatment has meant that for the majority of patients a normal life span and life style can be expected.
Almost any type of skin rash may occur. “Allergies” are common and indeed the lupus patient may give a history of allergies to drugs such as penicillin long before lupus has been diagnosed.
A pinkish rash on the cheeks is present in approximately one half of hospital patients – in fact the “classical” butterfly shaped rash is seen in a minority. Inflammation in small blood vessels of the skin may give rise to a variety of rashes – the most common is a pinkish spotty rash on the elbows and around the fingers and toes.
Patients with lupus may develop Raynauds phenomenon – a tendency for the fingers to go dead white then bluish on exposure to cold. This phenomenon, which may precede the diagnosis of lupus by many years, is, of course, not unique to SLE and is also seen in otherwise healthy individuals.
10. Thyroid problems
The thyroid hormones affect nearly all tissues of the human body, including the skin. Skin tissues contain thyroid hormone receptors which, when occupied by thyroid hormones, stimulate cellular activity.
Patients with hypothyroidism, or underactive thyroid disease, may experience skin symptoms that reflect diminished cellular skin activity in the absence of sufficient thyroid hormone. Some skin changes associated with hypothyroidism may cause rashes on elbow and itching around this area.
11. Skin Dryness and Scaling
Up to 90 percent of patients with hypothyroidism experience skin dryness and scaling, according to the medical textbook “Werner & Ingbar’s The Thyroid.”
When examined under the microscope, the skin of patients with hypothyroidism exhibits thinning and increased keratin, a protein found in the uppermost layer of the skin and in the hair and nails. The increased keratin and impaired shedding of old cells gives the skin a scaly appearance.
Rash on elbows does not itch
Psoriasis is a chronic skin condition thought to be caused by an immune system dysfunction. If you have psoriasis, your immune system sends signals to your skin that speed up the production of skin cells.
There are five types of psoriasis (plaque psoriasis, guttate psoriasis, pustular psoriasis, inverse psoriasis, and erythrodermic psoriasis), none of which is contagious. Each type causes a different skin rash and appears on different areas of the body.
It’s estimated that about 7.5 million Americans live with psoriasis. The condition does respond to treatment, but it may never go away completely and tends to come back. But because psoriasis can look like other skin conditions that cause itchy, scaly rashes with inflammation but these rashes don’t itch it is often confused with those disorders.
Rash on elbows and knees only
Psoriasis causes Itchy, red patches covered with silvery-white flaky skin. Common sites are the elbows and knees.
Discoid eczema is an allergy-related chronic skin condition. Discoid eczema is marked by itching, inflammation, redness, and scaling of coin-shaped patches on the skin. Discoid eczema is an uncommon type of eczema, a form of dermatitis.
Discoid eczema is also called nummular dermatitis and gravitational discoid eczema.
Discoid eczema causes rashes on the elbows and knees only and rarely do these rashes move to other areas of the body.
Rash on both elbows
Both elbows can get a bad rash. But what causes rashes on both elbows? Rashes can have many different causes and the specialists involved in diagnosis and treatment of the rashes includes general practitioners, general internists, dermatologists and rheumatologists.
A family history of rashes can help the clinician with coming up with a differential diagnosis of the causes of the rash. Rashes, are generally caused by immune mediated reactions that occur in our bodies.
Sometimes these reactions are caused by allergens that we expose our body to, other times they can be caused by autoimmune disorders such as psoriasis, lupus and rheumatoid arthritis which may present with symptoms like joint pain.
Other common causes of rashes can be caused by infectious processes such as viral and fungal infections as well as bites. Rashes can also be caused by taking medicines.
While a general practitioner can often make the diagnosis of a cause of a rash, sometimes it is appropriate to have a dermatologist or rheumatologist make the diagnosis, since sometimes rashes that are associated with systemic symptoms such as joint pain, vision and urinary symptoms can be more serious to treat and diagnose.
It is not possible to come to a diagnosis without a physical exam therefore evaluation by a physician is recommended.
Dry, itchy rash on elbows
Dry skin on your elbows may result from a variety of conditions, ranging from infections or boils to allergic reactions or dermatitis, according to the American Academy of Family Physicians.
Treatment varies from topical creams to medication and techniques to address the underlying cause of your dry skin.
Dermatitis is a skin condition that causes redness, swelling and itching — usually as a result of an allergy to certain fabrics or chemicals that touch your elbows. It causes your skin to break out in blisters and bumps that can be itchy and painful.
When the outbreaks occur primarily on your elbows, you may have a case of dermatitis herpetiformis. This condition is a side effect of gluten sensitivity or a reaction to products containing wheat. Antibiotics help control the dryness and itching
Rash on inner elbow or inside elbow
Eczema and psoriasis are distinct entities, and most dermatologists feel that the two do not exist at the same time in the same patient. That is not to say that they do not look alike, because they can.
They are both inflammatory conditions of the skin and, to some extent, they are treated similarly.
Eczema, specifically termed atopic dermatitis, is very common in children. With this condition, the littlest thing can induce redness and itching in the skin. (Eczema is uniformly more itchy than psoriasis.) The person then scratches the itchy spots, and characteristic red scaly patches develop.
Inside the elbow is a common location for eczema, not for psoriasis. Eczema likes to affect body parts that doctors call the “flexural surfaces” (neck, behind knees, inner elbows, etc.) whereas psoriasis likes the elbows, knees, scalp and belly button.
How to get rid of red rash on elbows
The most important thing when dealing with a rash is not to scratch it. Scratching will only aggravate the condition. Scratching in case of blisters will spread the rash to other skin areas and therefore avoid the same.
- Wash the affected area with cool water. If one wishes to use soap, then do not use any harsh soap but mild cleansers can be used. Do not wash the affected area more than 2 times in a day.
- If the affected area is itching too much, then apply ice compress to it. One can apply ice compress after every 1 or 2 hours, to soothe the elbow rash.
- To soothe the affected area, cut a leaf of aloe vera lengthwise, and apply the gel on the rash. Keep applying aloe gel 2-3 times a day. Aloe works very well to soothe burns, inflammation, rashes, dry skin, etc. We highly recommend organic cold pressed Aloe Vera (Check price on Amazon)
- Before going to bed, apply olive oil to elbow skin rash, with a cotton swab.
Sources and references:
- Beyond Celiac: Celiac Disease and Dermatitis Hypetiformis.
- London Lupus Centre: Lupus Symptoms on Skin.
- WebMD: Psoriasis-Understanding the Basics.