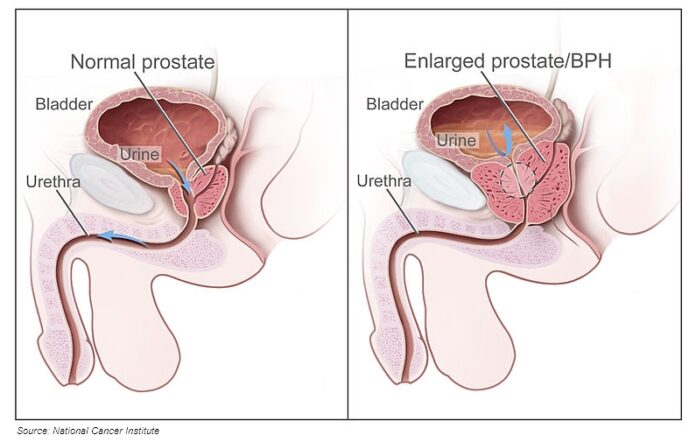
The prostate is a small, walnut-shaped muscular gland that can be found in the reproductive systems of those assigned male at birth (AMAB). The prostate’s main function is to produce the fluid that goes into semen, an essential substance for AMAB people’s fertility. The gland is located at the neck of the person’s bladder, surrounding the urethra, and helps propel prostate fluid and semen through the penis during ejaculation.
Sudden enlargement of the prostate is common for many people AMAB. This condition is most commonly known as benign prostatic hyperplasia (BPH), but it is also referred to as benign prostatic obstruction. It’s important to note that an enlarged prostate is not a sign of prostate cancer and doesn’t necessarily increase an affected individual’s chances of getting prostate cancer in the future.
While BPH is a noncancerous condition, it can give rise to uncomfortable symptoms and sometimes more severe complications in certain individuals. Fortunately, cases of BPH are treatable. Read on for a more comprehensive understanding of what causes BPH, what symptoms patients can expect, and how the condition can be treated.
Causes and Incidence of BPH
BPH is the most common prostate issue for people AMAB aged 50 and above. Although it’s rare for BPH to cause symptoms in patients aged younger than 40, symptoms are likely to both increase and become more frequent as the affected person ages. Roughly 50 per cent of people AMAB between the ages of 51 and 60 and as much as 90 per cent of people AMAB over 80 are likely to have BPH.
Although age is one of the primary determinants of a person’s risk for developing BPH, other factors can also contribute to raising that risk. For example, medical conditions such as type 2 diabetes, obesity, erectile dysfunction, and diseases of the heart and circulatory system can all raise a person’s chances of experiencing an enlarged prostate. A family history of BPH and a lack of physical exercise are also major contributing factors.
BPH is most commonly thought to be a natural product of ageing. Though its exact causes are currently unknown, one common theory is that BPH comes about as a result of changes in the levels of male sex hormones within the body.
Common Symptoms of BPH
Lower urinary tract symptoms are usually the first manifestations of BPH. These symptoms might include the following:
- Greater urinary urgency, or the inability to hold in one’s urine
- More frequent urination (8 times a day or more)
- Weak or interrupted urine streams
- Dribbling urine towards the end of urination
- Urine with unusual colours or smells
- Nocturia, or urination while sleeping
- Urinary incontinence
- Urinary retention
- Pain during urination or actual ejaculation
Symptoms of BPH typically occur when the urethra is blocked and the affected person’s bladder must then work harder to pass urine through the blockage. This blockage is not necessarily determined by the size of the prostate, as some people with significantly enlarged prostates experience little to no blockage at all. Others with minimally enlarged prostates, meanwhile, may experience greater blockage and therefore more symptoms.
More severe complications of BPH include the following conditions:
- Blood in the urine
- Urinary tract infections (UTIs)
- Acute (sudden-onset) urinary retention
- Chronic (long-lasting) urinary retention
- Bladder stones
- Kidney damage
- Bladder damage
Most individuals with BPH are unlikely to develop these complications. However, it’s still ultimately beneficial for anyone experiencing symptoms of BPH to seek medical care. The need for medical attention is especially urgent for individuals who experience the following symptoms:
- A painful, urgent, and frequent need to urinate, accompanied by chills and fever
- Blood in the urine
- A complete inability to urinate
- Severe pain or discomfort in the lower abdomen or the urinary tract
Diagnosis and Treatment of BPH
Doctors checking patients for BPH will typically start with a physical examination to estimate the size and shape of the prostate, as well as an interview about the patient’s medical history. A doctor may also recommend additional tests such as urinalyses, cystoscopies, urodynamic tests, and others. These tests will provide more detailed information on the state of the patient’s urine, urethra, and bladder.
Most treatment plans for BPH start with certain lifestyle adjustments aimed at mitigating the patient’s symptoms. For instance, doctors typically recommend that patients with BPH refrain from holding in their urine and instead urinate as soon as they feel the need. Some patients may also benefit from going to the bathroom to urinate even if they have no urge to do so immediately.
Other lifestyle changes that can help mitigate BPH symptoms include the following:
- Regular exercise
- Doing Kegel exercises to fortify the pelvic muscles and facilitate easier urination
- Reducing stress levels
- Avoiding caffeine and alcohol, particularly in the evening
- Avoiding over-the-counter decongestants, antihistamines, and other medications that may make it more difficult to empty the bladder
If the above lifestyle changes aren’t enough to relieve a patient’s BPH systems, doctors may recommend certain medications, such as antibiotics, alpha-1 blockers, or hormone-reduction medications. Some of these medicines may relieve the symptoms of BPH, while others focus on reducing the size of the prostate itself. For cases of BPH that don’t resolve themselves with medication, surgery is often recommended.
While BPH doesn’t always require aggressive medical treatment, it’s always a good idea for patients with the condition to monitor their symptoms and check in with their doctors frequently. A doctor’s professional perspective is necessary for developing BPH treatment plans that are tailored to the unique needs and situations of individual patients.